Does Draining an Abscess Hurt? Pain, Procedure, and Aftercare
Explore whether draining an abscess hurts, what the procedure involves, expected discomfort, postprocedure care, and when to seek professional help with guidance from Drain Guide.
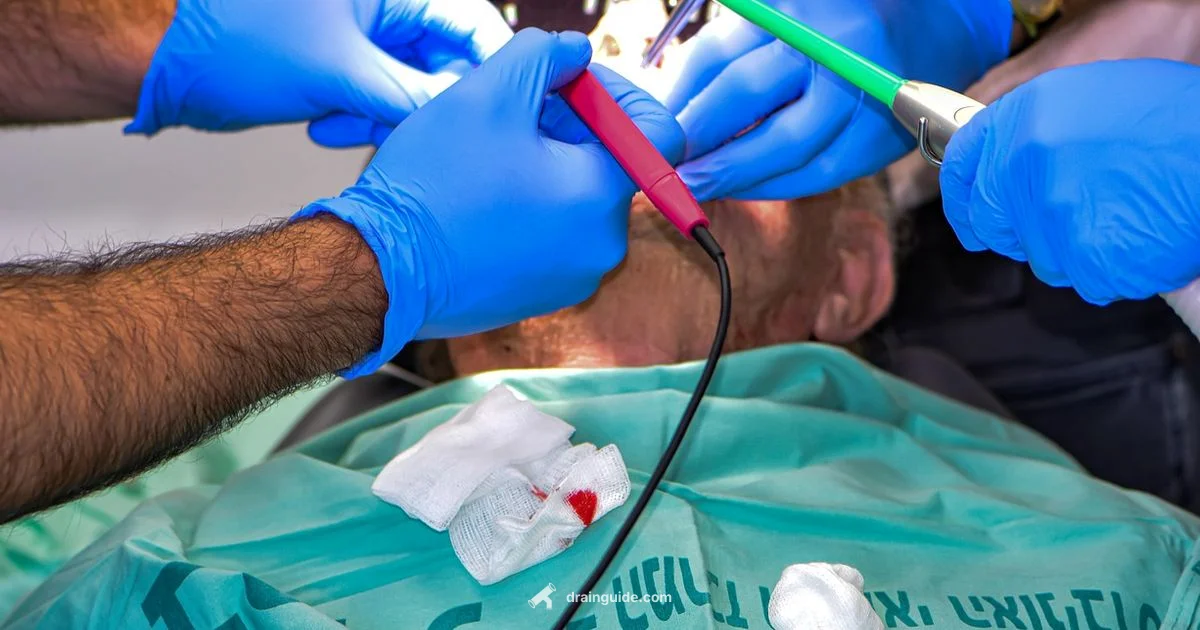
Abscess drainage is the medical procedure of releasing pus from an infected pocket under the skin to relieve pressure and promote healing.
What is an abscess and what does drainage involve?
An abscess forms when bacteria invade tissue, creating a pocket of pus surrounded by inflamed skin. Drainage is the medical procedure used to release that pus, relieve pressure, and kickstart healing. Abscess drainage is typically performed by a clinician using sterile technique and local anesthesia. According to Drain Guide, understanding the nature of the abscess helps you anticipate what happens next and what to expect in terms of pain and recovery. If you are wondering does draining an abscess hurt, most people report a brief sting when the local anesthetic is applied, followed by milder discomfort during the procedure. The goal is to remove pus and debris, then allow the site to heal. Abscesses occur most commonly in skin but can form deeper in the body, requiring more careful planning and sometimes imaging to guide drainage. The decision to drain hinges on the size, location, risk of rupture, and signs of infection such as spreading redness or fever.
Does draining an abscess hurt during professional care and how pain is managed
Pain during professionally performed drainage is typically minimized with local anesthesia. A clinician numbs the skin and underlying tissue before making a small incision or creating a tract for drainage. The experience is usually described as a brief sting as the anesthetic is injected, followed by only mild to moderate discomfort during drainage. The procedure is performed with sterile technique to reduce infection risk, and pain management can be adjusted if you express concern. Aftercare, pressure relief, and drainage of the pocket can be tolerable, and your clinician can switch anesthesia or timing if needed. Pain often subsides as healing begins. In many cases, soreness lasts a day or two, and clinicians may recommend over the counter pain relief and warm compresses to comfort the area.
Home drainage versus professional care: why professional care is recommended
DIY drainage is dangerous and not advised. Attempting to drain an abscess at home can spread infection, push material into surrounding tissue, or cause tissue damage, leading to worse scarring or systemic illness. If you notice an abscess, the safest approach is to seek professional care promptly. Signs that an abscess may require urgent evaluation include increasing redness, fever, swelling spreading beyond the area, or a rapidly enlarging lump. A clinician can assess the abscess, determine whether drainage is appropriate, and perform it under sterile conditions, often with imaging guidance for deeper pockets. Drain Guide emphasizes that proper assessment and technique reduce complications and improve healing outcomes.
Aftercare and wound management after drainage
Postdrainage care focuses on keeping the site clean, protecting it from trauma, and monitoring for signs of infection. Follow your clinician’s instructions for dressing changes, wound cleansing, and activity limitations. Generally you should wash gently with mild soap, avoid picking at the wound, and keep the area dry during initial healing. Change dressings as advised and watch for redness, swelling, warmth, or foul discharge. If prescribed antibiotics, take them as directed to prevent reinfection. Pain can usually be managed with simple remedies as advised by your clinician. By maintaining proper hygiene and allowing the tract to drain appropriately, most abscess wounds heal in expected time frames. Drain Guide notes that consistent aftercare significantly lowers complication risks.
Risks, complications, and red flags to watch for
While drainage is a common and effective treatment, it carries risks. These include recurrence of the abscess, persistent infection, or delayed wound healing if aftercare is missed. Rare complications can include spreading infection or damage to nearby tissues, especially with deep abscesses. Watch for red flags such as fever, worsening pain, spreading redness, increasing swelling, or foul discharge. Seek urgent care if symptoms worsen or you feel unwell.
Practical tips for preparing and talking with your clinician
- List your symptoms, how long they have persisted, and any previous abscess episodes.
- Ask about anesthesia options, expected pain, dressing choices, and follow‑up plans.
- Understand the antibiotic plan if one is prescribed and any drug interactions to avoid.
- Bring a list of questions to help you feel prepared and informed.
- Aftercare checklists and warning signs to watch for should be reviewed before discharge.
The Drain Guide team recommends asking about aftercare specifics and ensuring you have clear instructions to minimize pain and infection risk.
Got Questions?
Does draining an abscess hurt?
Pain varies, but professional drainage usually involves a brief initial sting from anesthesia followed by limited discomfort. Clinicians tailor pain control to your needs, and most people recover with minimal ongoing pain.
Yes, there can be some pain, especially during the initial numbing, but it’s generally brief and well controlled by the clinician.
How long does abscess drainage take?
The procedure is typically quick when performed by a clinician, often under an hour depending on the abscess size and location. Your clinician will give you a more precise timeframe.
It’s usually a short procedure, with timing depending on the abscess. Your clinician can tell you what to expect.
Are antibiotics always needed after drainage?
Antibiotics are not always required after drainage. They may be prescribed if there are signs of systemic infection, extensive surrounding infection, or if the abscess is deep or recurrent.
Antibiotics aren’t always necessary after drainage; your doctor will decide based on the infection’s severity.
Can I drain an abscess at home?
Home drainage is not recommended. It can spread infection, cause tissue damage, and lead to complications. Seek professional care for a safe evaluation and drainage if needed.
No. Do not attempt to drain at home. See a healthcare professional for proper treatment.
What signs mean I should seek urgent care after drainage?
Seek urgent care if you develop fever, increasing redness or swelling, worsening pain, spreading redness beyond the wound, or foul discharge.
If fever or worsening symptoms appear, contact a clinician promptly for evaluation.
What should I ask my clinician before drainage?
Ask about anesthesia options, expected pain, wound care, dressings, activity limits, and follow up. Clarify when to return for review or dressing changes.
Ask about pain control, aftercare, and follow up so you’re clear on the plan.
The Essentials
- Prepare with clear questions for your clinician
- Pain is generally controlled with local anesthesia
- Professional drainage is safer than DIY attempts
- Follow wound care instructions to reduce infection risk
- Watch for red flags and seek care promptly