What Is Drainage From a Wound A Practical Home Guide
A practical guide to wound drainage, covering what it is, how to recognize healthy versus problematic drainage, warning signs of infection, and safe home care steps. Learn to distinguish normal healing fluids from concerns requiring medical advice.
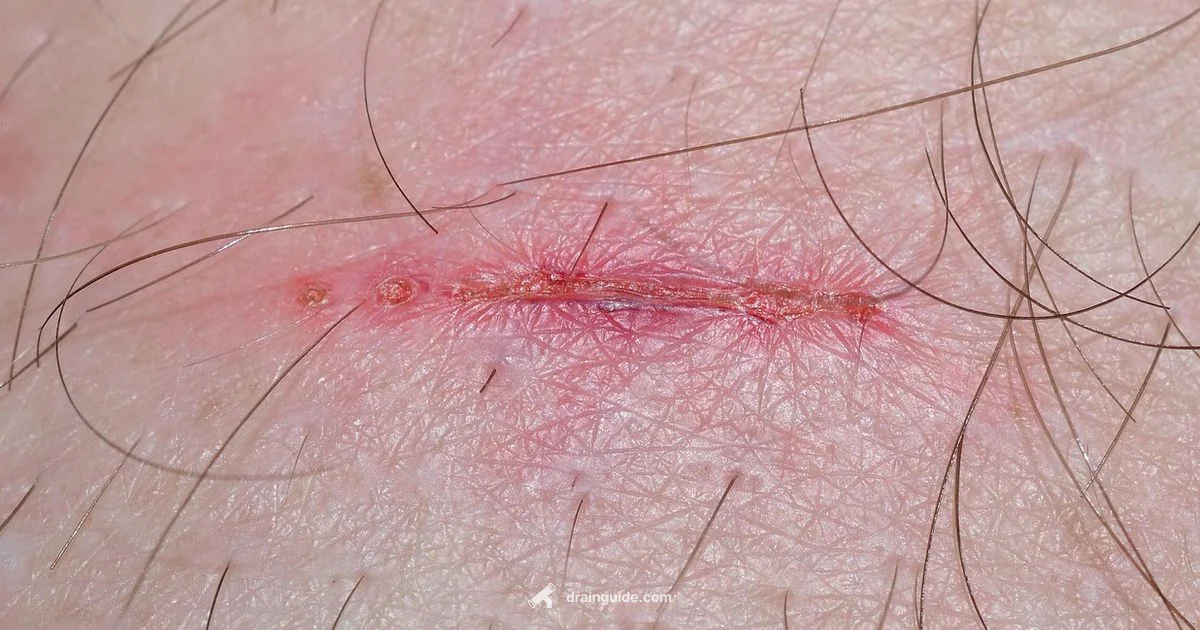
Drainage from a wound is the fluid that leaks from damaged skin during healing. It can include serum, blood, and pus; its appearance and amount can indicate normal healing or a potential infection.
What is drainage from a wound?
Drainage from a wound is the fluid that leaks from damaged skin during healing. It can include serum, blood, and occasionally pus; its appearance and amount can indicate normal healing or a potential infection. According to Drain Guide, understanding these fluids helps homeowners distinguish between healthy progress and complications. In most cases, drainage is a sign that the body is repairing tissue and removing debris. The color, consistency, and volume change as healing progresses, so noting patterns over several days is more informative than a single observation.
Healthy drainage is usually clear to pale yellow and slightly watery early on, steadying as the wound closes. If you notice a sudden increase in drainage, a dramatic color change, a strong odor, or increasing pain, it may signal a problem and deserves closer attention from a clinician.
Types of wound drainage
Wound drainage comes in several forms, and recognizing the difference helps guide care:
- Serous drainage: clear or pale yellow and watery; common in early healing and typically harmless when in limited amounts.
- Sero-sanguineous drainage: pink to light red and thin; a mix of serum and blood often seen after an injury or after procedures.
- Purulent drainage: thick, cloudy, may be yellow, green, or brown and can have an odor; this type may indicate infection or contamination. Each type provides clues about healing progress and the need for changes in dressing or medical evaluation.
Normal healing versus warning signs
During healing, it is normal for drainage to fluctuate in amount and color. A gradual decrease over days, the absence of foul odor, and diminishing redness around the wound site generally indicate progress. Red flags that warrant medical advice include heavy drainage that soaks through dressings quickly, a strong or foul odor, increasing redness or swelling around the wound, fever, or drainage that becomes purulent. If the skin over the wound shows warmth or tenderness that worsens, contact a clinician promptly.
Documenting daily observations helps distinguish normal variation from a pattern that suggests infection or contamination. If you have underlying conditions, such as diabetes or immune suppression, err on the side of caution and seek care earlier rather than later.
How clinicians assess drainage in a wound
Healthcare professionals assess drainage by looking at color, consistency, odor, and volume, then compare these observations against the wound’s stage of healing. They may use sterile swabs to collect samples for basic testing if infection is suspected. Imaging or clinical signs, such as fever or spreading redness, contribute to the overall assessment. It is important to keep the wound clean and follow prescribed dressing protocols so that the clinician can accurately evaluate healing progress without commentary from home care products or improvisation.
Home care steps to manage drainage safely
Safe home care focuses on keeping the wound clean, protecting it from contamination, and choosing appropriate dressings that absorb excess fluid. Start with clean hands and follow the care plan provided by your clinician. Use mild soap and water or saline for gentle cleansing, then apply a clean, breathable dressing that matches the drainage level. Change the dressing when it becomes wet or soiled, and avoid reusing cotton fibers or lint that can shed into the wound. If you notice persistent drainage despite proper dressing, or if symptoms worsen, contact your healthcare provider for guidance.
Keeping a log of changes in drainage color, amount, and odor can help you and your clinician decide whether the current care plan is effective or needs adjustment.
Red flags and when to seek medical attention
Call your clinician or seek urgent care if you observe any of the following: drainage that is heavy or rapidly increasing, purulent odor, continuous fever, spreading redness, severe pain, or wound edges that separate. In cases of deep wounds, puncture injuries, or wounds with compromised blood flow, a professional evaluation is advised even if drainage seems manageable at home. If you have diabetes, vascular disease, or a weakened immune system, err on the side of caution and consult a clinician sooner rather than later.
Authority sources and safety tips
For reliable guidance on wound care and drainage, consult trusted health authorities. Consider reviewing general wound care resources from reputable organizations to supplement home care instructions:
- https://www.nhs.uk/conditions/wounds/
- https://www.cdc.gov
- https://www.nih.gov
Safety tip: never apply unproven remedies or “home remedies” that could irritate the wound or introduce pathogens. Always follow the specific instructions from your clinician and report any concerning changes promptly.
Got Questions?
What causes drainage from a wound?
Drainage is produced by the body during inflammation and healing. It can be a normal part of tissue repair but becomes concerning if it is heavy, purulent, foul smelling, or accompanied by fever or spreading redness.
Drainage comes from the body’s healing response. If it’s heavy or smells bad, seek medical advice.
What does normal drainage look like at different healing stages?
Early in healing, drainage tends to be clear or pale yellow and may be thin. Over time it should become lighter and reduce in amount. Any sudden change to thick, colored, or foul drainage is a warning sign.
Early on it may be clear and watery, then it should lessen in amount and clarity as healing progresses.
When should I seek medical care for drainage?
Seek care if drainage is heavy, purulent, foul, or if you develop fever, increasing pain, or redness around the wound. Also consult if you have a chronic condition that affects healing.
If drainage is heavy or foul or you have fever or growing redness, see a clinician.
Can you prevent drainage problems at home?
Yes. Keep the wound clean and dry, change dressings promptly, wash hands before touching the wound, and follow your clinician’s instructions. Avoid irritants and monitor for changes daily.
Keep it clean, dry, and covered and watch for warning signs.
What supplies help manage drainage at home?
Use appropriate dressings recommended by your clinician, sterile saline or mild cleansers for cleaning, and clean, nonfibrous materials for covering the wound. Avoid old dressings and improvisation with nonsterile items.
Have the right dressings and cleansers ready and replace them as advised.
Is drainage always a sign of infection?
Not necessarily. Drainage can be part of normal healing, but purulent drainage with odor or fever can indicate an infection. When in doubt, ask a clinician for an evaluation.
Drainage does not always mean infection, but certain changes do require medical advice.
The Essentials
- Know the three common drainage types and what they mean
- Monitor color, odor, and volume of drainage daily
- Change dressings safely and seek care for red flags promptly
- Document changes to share with your clinician
- Avoid unproven home remedies and follow professional guidance