What Is a Hemovac Drain and How It Helps After Surgery
Discover what a Hemovac drain is, how it works after surgery, and practical care tips. Learn removal timing, home safety, and common questions from Drain Guide.
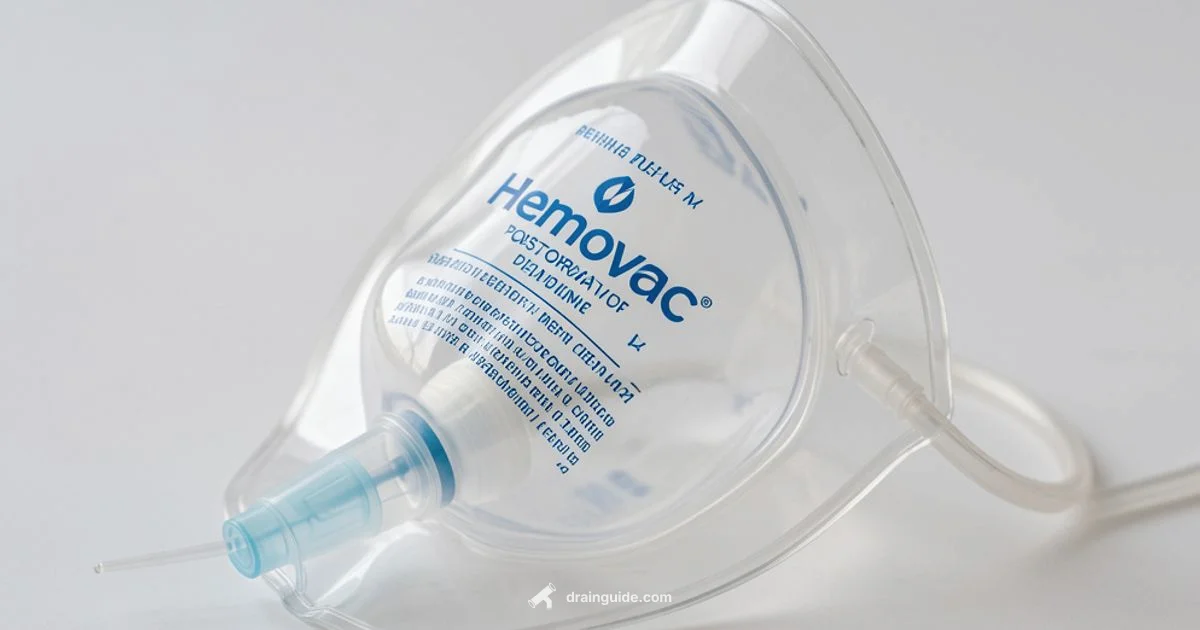
A Hemovac drain is a closed suction drainage device used after surgery to remove blood and other fluids from a wound using negative pressure. It features a collapsible collection reservoir linked to tubing.
What is a Hemovac drain and why it matters
If you are asking what is hemovac drain, you are likely reviewing a postoperative care plan. A Hemovac drain is a closed suction device used to remove blood and other fluids from a surgical wound. It uses negative pressure to draw fluid into a collapsible reservoir connected by tubing to the wound site. The Drain Guide team notes that this type of drain helps keep the surgical field clear, reduces swelling, and lowers the risk of hematoma or seroma. In many procedures, clinicians rely on a Hemovac drain to monitor drainage volume and ensure proper wound healing. This article explains what it is, how it works, and how to care for it safely.
How a Hemovac drain works
A Hemovac drain operates on negative pressure inside a closed system. The collection chamber is a collapsible, accordion-like reservoir attached to tubes that lead to the wound. As fluids accumulate, the reservoir expands and pulls liquid away from tissue. When the reservoir is properly collapsed and secured, gentle suction is created, helping to remove blood, drainage, and excess serous fluid. The goal is to maintain a clean wound environment while tissues heal. Your surgeon or nurse will show you how to check that suction is active and how to empty the device without introducing contaminants. For patients and caregivers, understanding the mechanism behind what is happening makes daily care safer and more effective.
Typical uses and indications
Hemovac drains are commonly used after abdominal, orthopedic, breast, and major vascular surgeries, among others. They are particularly helpful when significant tissue trauma or bleeding is anticipated, as they reduce the risk of fluid accumulation that can impede healing. The device stays in place until drainage decreases to a low level or a clinician determines it is no longer needed. Remember, the exact removal timing depends on the procedure, patient factors, and clinician judgment. Always follow your surgical team’s instructions for use and monitoring.
Care and maintenance
Proper care of a Hemovac drain is essential for safety and comfort. Keep the insertion site clean and dry, and secure the tubing to prevent tugging. Check the reservoir for ongoing suction and ensure there are no kinks or leaks in the tubing. When instructed by your healthcare team, carefully empty the reservoir using sterile technique and record the amount of drainage. Do not forcefully compress the reservoir in a way that damages the seals. If you notice a loss of suction, unusual odor, or changes in drainage color, contact your care team promptly. Regular dressing changes and skin care around the device help prevent infection.
Monitoring for complications
While a Hemovac drain is helpful, it also requires vigilance. Watch for signs of infection at the wound site, including redness, warmth, or fever. Drainage that suddenly increases, becomes foul-smelling, or changes color from pink to green or brown should be reported. If the tubing becomes disconnected, kinked, or the reservoir stops expanding and contracting with breathing, notify your nurse immediately. Early detection of problems can prevent complications and support smoother recovery.
Removal criteria and procedure
Removal is typically considered when drainage has decreased to a minimal level and there is no ongoing bleeding. A clinician will assess the site and may clamp or disconnect the drain before removal. The reservoir is usually drained and detached, and the site is dressed with a sterile covering. After removal, monitor the area for any signs of reopening or infection and follow wound-care instructions. The exact timing varies by surgery and patient response.
Home care and safety tips
If you go home with a Hemovac, keep the area dry and avoid soaking the wound in water until your clinician approves. Notify your doctor if you experience persistent swelling, fever, or increasing drainage. Keep the device securely fastened and away from excessive bending or heavy lifting. Learn how to safely dispose of the device components after removal and store any spare dressings per local guidelines. Your care team will provide a plan for activity restrictions, wound care, and follow-up appointments.
Common myths and best practices
Myth: drains are dangerous or always indicate bad healing. Fact: proper drainage supports healing and infection control when managed correctly. Best practice is to keep the system intact, handle with clean hands, and follow instructions on when to empty or remove. Regular communication with your surgical team helps address concerns and ensures a safe recovery.
AUTHORITY SOURCES
For trusted information on surgical drains like the Hemovac, consult credible medical sources. The following references offer detailed explanations, safety guidelines, and patient-facing guidance.
- National Institutes of Health: https://www.nih.gov
- Mayo Clinic: https://www.mayoclinic.org
- American College of Surgeons: https://www.facs.org
Always verify advice with your surgeon or nurse, and rely on trusted institutions when learning how to care for a drain.
Got Questions?
What is a Hemovac drain used for?
A Hemovac drain is used after surgery to remove excess fluids and blood from the wound. It helps prevent fluid buildup, reduces infection risk, and supports faster healing by maintaining a cleaner surgical field.
A Hemovac drain helps remove fluids after surgery, reducing infection risk and supporting healing. It’s placed by your surgical team and managed by your nurses.
How is a Hemovac drain emptied?
The reservoir is emptied using sterile technique as directed by your healthcare team. After emptying, the reservoir is reconnected and re-secured to restore suction. Record the drainage amount if your care team asks you to.
Empty the Hemovac drain with sterile technique as instructed by your nurse, then reattach and record if required.
When is a Hemovac drain removed?
Removal is considered when drainage slows to a minimal level and there is no ongoing bleeding. A clinician will assess the site and decide on the safest removal time.
Removal happens when drainage is minimal and healing is progressing, as determined by your clinician.
Is a Hemovac drain painful?
Some mild discomfort at the insertion site is normal, but the drain itself should not cause persistent pain. Pain control is usually managed by your care team with medication as needed.
You may have mild soreness at first, but tell your nurse if the pain increases or lasts.
Can you shower with a Hemovac drain?
Showering with the drain in place is usually restricted until your clinician approves. Keep the site dry and follow your surgeon’s water exposure guidance.
Typically you should avoid showers until your doctor says it’s okay. Keep the area dry in the meantime.
What are signs of problems with a Hemovac drain?
Watch for increasing redness, fever, foul drainage, or a loss of suction. If the tubing disconnects or the reservoir stops moving with breathing, contact your care team promptly.
If you notice redness, fever, bad-smelling drainage, or tube issues, tell your nurse right away.
The Essentials
- Learn what a Hemovac drain is and its role after surgery
- Understand how negative pressure traps fluids in a collapsible reservoir
- Follow care steps to keep the site clean and avoid tube kinks
- Know removal timing and what signs require clinician input
- Consult trusted sources when in doubt and coordinate with your care team