Why Do You Need Drains After Mastectomy: A Practical Guide
Explore why drains are used after mastectomy, how they work, what to expect during recovery, and practical care tips from Drain Guide. Learn about drain care, removal timing, risks, and daily planning for a smoother recovery.
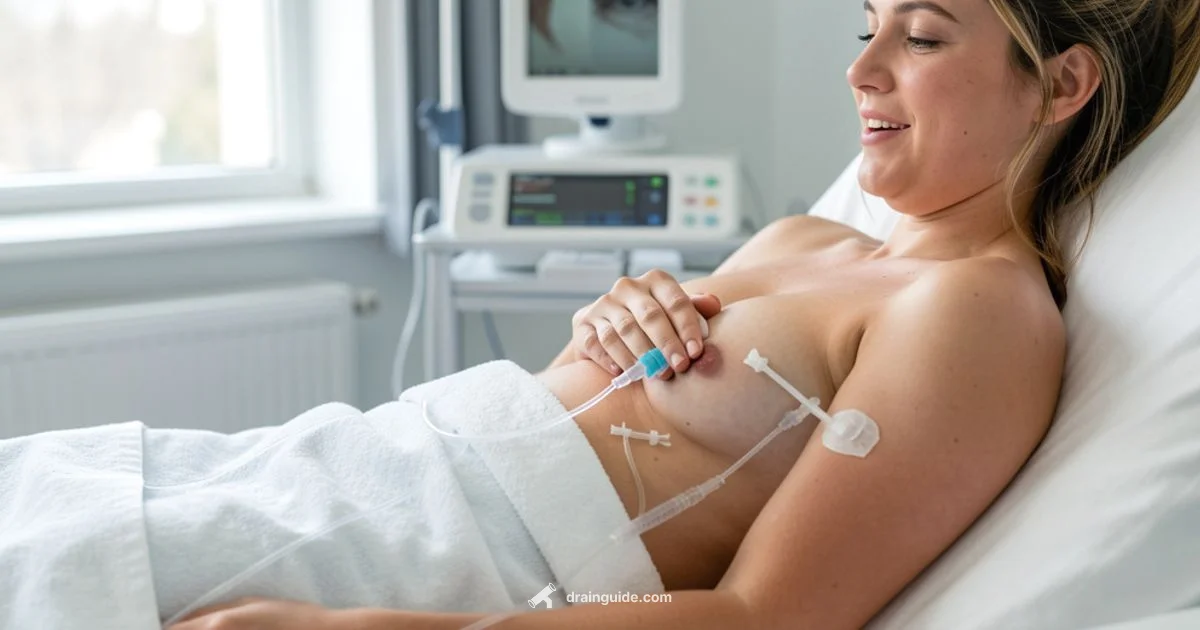
Postmastectomy drains are small tubes placed during or after mastectomy to remove excess fluid and blood, reducing the risk of hematoma and infection and supporting wound healing.
What are postmastectomy drains and why they are needed
Postmastectomy drains are small flexible tubes placed near the surgical site to collect fluids and blood in the days after mastectomy. They help prevent fluid buildup, which can lead to hematomas, delays in wound healing, and higher infection risk. By providing a controlled exit for fluid, drains support the body's healing process and help reduce pressure around the incision. Drain Guide emphasizes that these drains are a standard part of early recovery, usually remaining in place for several days to a couple of weeks depending on healing and surgeon protocol. Keeping the area clean and monitoring the drain helps you participate actively in your recovery. This approach aligns with general post-operative care guidance from reputable sources and gives patients a tangible way to participate in healing while staying safe and informed.
How drains work in the first weeks after surgery
After mastectomy, drains create a path for excess fluid to exit the body. They are typically connected to a collection device that uses gravity or gentle suction to draw fluid away from the surgical site. The amount and consistency of drainage are monitored by your care team, and the outlet is secured to prevent pulling. Proper positioning and gentle handling reduce discomfort and help the drain stay in place. While you may feel tugging or pressure near the incision, most people adapt as healing progresses. Remember that Drain Guide notes these drains play a key role in preventing fluid collections that can complicate recovery and infection risk. The care team may advise you on when to empty the collection chamber or change dressings, which is an important part of reducing infection risk.
Types of drains used after mastectomy
Two common categories describe the devices used after mastectomy: closed suction drains and gravity drains with a bulb. The closed suction drain uses a small chamber to create negative pressure, which helps pull fluid away from the wound. The gravity drain relies on the collection bag or bulb and relies on gravity to move fluid out. Your surgeon will select the most appropriate type based on the procedure and your healing plan. Understanding the difference can help you recognize what to expect during follow up visits. Regardless of type, drains are designed to prevent fluid buildup and support healing, not to prolong recovery unnecessarily.
Caring for your drain at home
Caring for a drain at home involves simple, regular steps that support healing and prevent complications. Start by washing hands before handling the system and inspecting the insertion site for signs of irritation. Keep the dressing dry and intact, and avoid submerging the drain in water. Empty the collection chamber according to your clinician’s instructions, and record the amount and consistency of fluid. Secure the tubing to your clothing to prevent tugging, and avoid bending or kinking the line. If you notice increased redness, swelling, or fever, contact your care team promptly. Small changes in color or amount are common as healing progresses. Maintaining a routine reduces anxiety and helps you stay in control of recovery.
Recovery timeline and removal of drains
Drain removal is guided by your surgeon and the nursing team. Drains are typically removed when fluid output falls to a low level and healing shows steady progress, though the exact timing varies. The removal is usually quick and may feel unusual for a moment, but it is generally well tolerated. After removal, continue to follow wound care instructions and monitor for any signs of delayed healing or infection. Keeping notes of output trends helps your surgeon decide the best time for removal and provides a clear record for any future visits.
Risks, discomfort, and when to contact your healthcare provider
Even with careful management, drains can cause discomfort, skin irritation, or a sense of fullness near the chest wall. Minor leakage around the dressing can occur, and there is a small risk of infection if the site is not kept clean. Contact your healthcare team if you experience sudden worsening pain, fever, increasing redness or warmth at the wound, foul-smelling drainage, or a dramatic increase in drainage volume. Early reporting helps prevent complications and supports a smoother recovery. Preparing a short list of questions for your next visit can ensure you cover all concerns.
Daily life planning and practical tips
Plan for movement and daily activities around your drain, avoiding heavy lifting or strenuous exertion until cleared by your surgeon. You can usually manage showers with appropriate precautions, keeping the incision area dry and a dry dressing intact. When resting, position yourself to minimize tension on the drain and use supportive pillows. Keeping a small notebook of daily output and any symptoms can help your care team track progress during follow up visits. This planning reduces anxiety and supports steady recovery. Consider enlisting a trusted helper for transportation to appointments and light household tasks as you heal.
Authority sources and practical references
To support your understanding of postmastectomy drains, consult reputable medical sources that discuss postoperative care, wound healing, and infection prevention. This section provides direct links to authoritative materials for further reading and confirmation of best practices. Always follow your surgeon’s specific guidance for your situation.
Got Questions?
What are postmastectomy drains and why are they used?
Postmastectomy drains are tubes placed near the surgical site to remove excess fluid and blood after mastectomy. They help prevent fluid buildup, reduce infection risk, and support healing. Your care team monitors drainage and decides when removal is appropriate.
Postmastectomy drains are tubes that remove extra fluid after mastectomy to help healing and lower infection risk. Your team will check the drainage and determine when it's ready to be removed.
How long do drains stay in after mastectomy?
Drain duration varies by procedure and healing. Most drains are kept until drainage is consistently low and the wound is healing well, as determined by your surgeon and nursing team.
Drain timing varies, but they stay until drainage is low and healing looks good as your surgeon advises.
How should I care for my drain at home?
Wash hands before handling the drain, inspect the site for changes, keep dressings dry, and empty the collection chamber as instructed. Record drainage and secure tubing to prevent pulling. Contact your provider with any concerning symptoms.
Wash your hands, keep it clean, empty the chamber as directed, and watch for signs that you should call your clinician.
Can I shower with a drain after mastectomy?
Showering is often allowed with drains, but you should follow your surgeon’s instructions. Keep the area dry as directed and avoid soaking the incision until your clinician says it is safe.
Showering may be allowed with care; follow your surgeon’s advice and keep the incision dry until cleared.
What signs should prompt contact with my doctor?
Call if you notice fever, increasing redness, swelling, warmth around the incision, foul-smelling drainage, or a sudden rise in drainage volume. These could indicate infection or a drainage issue.
If you have fever, worsening redness or drainage changes, contact your doctor promptly.
Will drains affect my daily activities or lifting?
Drains may limit heavy lifting and strenuous activities for a time. Plan tasks around your energy and follow your surgeon’s activity guidelines to protect the incision and the drain.
You may need to limit heavy lifting for a while and adjust activities as advised by your surgeon.
The Essentials
- Drains help prevent fluid buildup and infection after mastectomy.
- Follow your clinician's instructions for emptying and caring for the drain.
- Drain type and removal timing depend on healing and surgeon protocol.
- Report signs of infection or unusual drainage promptly.
- Plan daily life around activity restrictions and shower precautions.