Penrose Drain Guide: Definition, Uses, and Care
Penrose drains explained: what they are, how they work, when they’re used, and essential care tips for caregivers and patients.
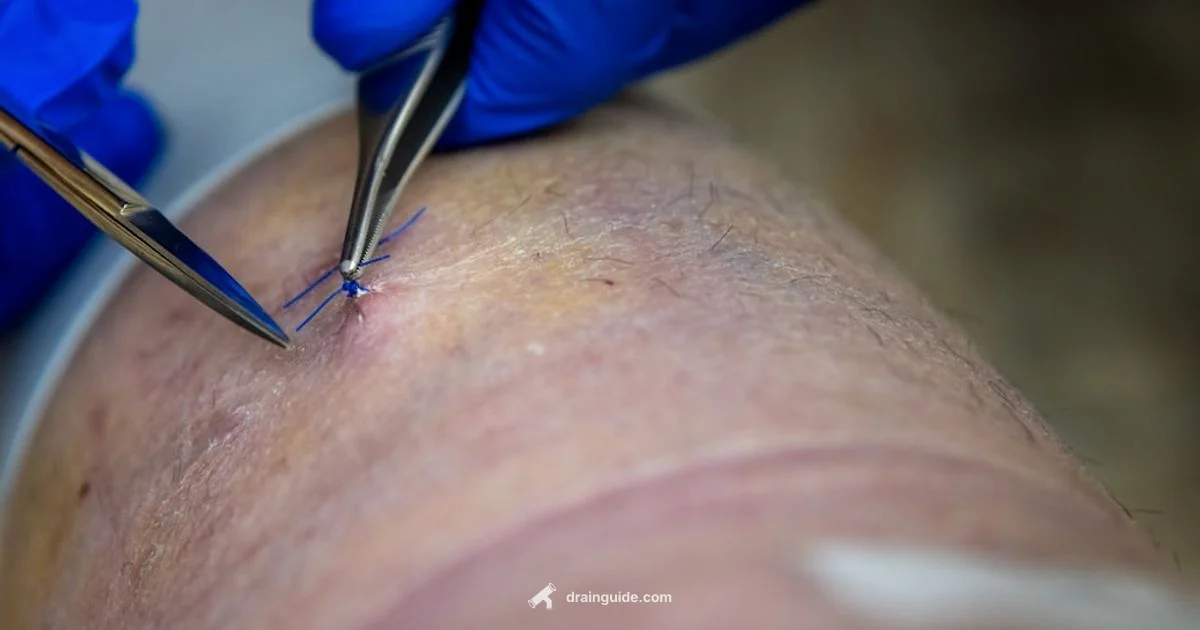
Penrose drain is a soft, flexible rubber tube placed in a wound to allow passive drainage by gravity.
What is a Penrose Drain?
A penrose drain is a soft, flexible rubber tube used to help a wound drain fluid and pus by gravity. It is a simple, low-cost device that has been a staple in wound care for many decades. According to Drain Guide, penrose drains provide passive drainage without active suction, relying on the natural movement of fluids to exit the wound and surrounding dressing. While the term is sometimes capitalized as Penrose drain, the lowercase form penrose drain is commonly used in patient education materials. In practice, the tube exits the wound through a small opening in the dressing and travels to a safe exterior area where drainage collects. The goal is to prevent fluid buildup, reduce pressure on tissues, and promote healing by keeping the wound environment clean and drained. This type of drain is typically indicated for wound cavities, abscess drainage, or the temporary management of fluid after certain surgical procedures.
In clinical settings, the exact placement and length are determined by the surgeon or wound care specialist. The penrose drain is usually secured to prevent accidental removal, and it may be connected to a dressing that helps keep the exit site clean. It remains in place under professional supervision until drainage decreases and the wound shows signs of healing. While not every wound requires a drain, penrose drains are valued for their simplicity, low cost, and versatility in a variety of soft tissue infections and postoperative scenarios. Drain Guide notes that patient education around drainage monitoring and dressing changes is essential for reducing complications and ensuring safe healing.
How a Penrose Drain Works
A penrose drain operates on a straightforward principle: gravity-driven drainage through a soft rubber tube creates an exit path for accumulating fluids. Unlike active suction devices, it relies on the weight of gravity and capillary action to move fluid from the wound cavity to the exterior dressing. The exterior portion of the tube is secured so it does not shift and cause discomfort or accidental dislodgement. In most setups, there is no attached collection canister; instead, the drainage is absorbed by dressings surrounding the exit site. This makes penrose drains a lightweight option that can be tailored to the wound’s size and shape. When a drain is placed properly, the wound cavity remains decompressed, which can support tissue repair and reduce dead-space that can harbor infection. Practitioners assess the appearance and amount of drainage to gauge healing progress and determine when to remove the drain. Drain Guide emphasizes routine monitoring, including checking the color, consistency, and odor of drainage, as well as any changes in surrounding skin.
Got Questions?
What is a penrose drain and how does it differ from other surgical drains?
A penrose drain is a soft rubber tube used for passive drainage by gravity. Unlike active suction drains, it does not require a powered mechanism to remove fluid; instead, fluid drains along the outside of the tube into a dressing. It is commonly used for wound cavities or after certain procedures to prevent fluid buildup.
A penrose drain is a soft rubber tube that drains wound fluid by gravity, without suction. It helps keep pressure down and supports healing under doctor supervision.
When is a penrose drain typically used?
Penrose drains are typically used after surgical procedures or for wound infections involving cavities where fluid buildup could delay healing. They help prevent accumulation of pus or serous fluid and reduce the risk of pressure on nearby tissues. Decisions about use depend on the surgeon’s assessment.
It’s usually used after surgery or in wounds where fluid buildup would slow healing, as determined by a clinician.
How long does a penrose drain stay in place?
The duration varies with the wound’s healing rate and the amount of drainage. Most drains are removed when drainage decreases to minimal levels and the wound shows clear signs of healing. Only the supervising clinician should decide removal timing.
Removal timing depends on healing progress and drainage levels, decided by the clinician.
What are signs of trouble with a penrose drain?
Watch for increased redness, swelling, fever, foul-smelling drainage, changing color of drainage to bright red, or a drain becoming dislodged. If you notice any of these signs, contact the treating clinician promptly.
Seek medical advice if you see redness, fever, foul drainage, or if the drain looks loose.
Can a penrose drain be managed at home?
Care should be guided by a clinician. You can perform basic dressing care and monitor drainage, but do not attempt to adjust or remove the drain yourself. Seek professional guidance for any concerns or changes in symptoms.
Basic dressing care is okay, but any drain adjustments require a clinician.
The Essentials
- Penrose drains provide passive, gravity-driven drainage.
- Only trained clinicians should insert or remove them.
- Monitor the exit site for redness, swelling, or unusual drainage.
- Report changes like sudden pain, leakage, or dislodgement promptly.
- Discuss alternatives with your clinician if unsure about the best option.