What Kind of Drain Is Used for Abdominal Surgery
Explore the common drains used after abdominal surgery, how doctors choose them, how to care for a drain, and what to expect during removal.
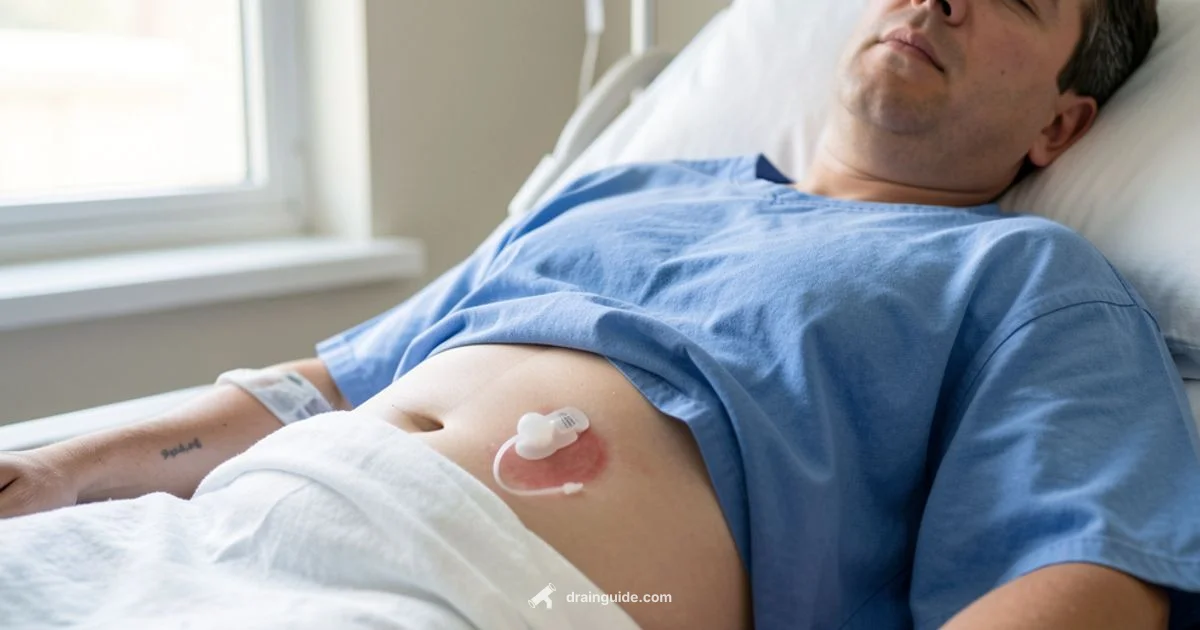
An abdominal surgical drain is a temporary tube placed during abdominal surgery to remove fluids or air from the peritoneal cavity, helping prevent accumulation and infection.
What is an abdominal surgical drain and why it's used
A surgical drain is a tube inserted into or near the operative area to remove fluids such as blood, pus, or serous fluid, and sometimes air. In abdominal surgery, drains help prevent fluid collections that can delay healing or lead to infection. They also provide a way for clinicians to monitor the healing process by observing the volume and composition of what drains out. Not every abdominal operation requires a drain; the decision depends on the procedure, tissue handling, and expected fluid production.
According to Drain Guide, the use of a drain is individualized and based on factors like the extent of dissection, risk of fluid accumulation, and tissue stability. Drains are typically positioned to exit through a small incision away from the main wound, connected to a collection system that can operate by gravity or suction. While drains add a step to the recovery process, they are intended to shorten complications and improve monitoring in the immediate post operative period. Removal generally occurs when healing progresses and drainage decreases to a level deemed safe by the surgical team.
In most cases, patients notice the drain as a soft tube leaving the body with a small dressing. The drain site is cared for much like a wound, and caregivers provide instructions on how to keep it clean and secure while avoiding tugging or daily activity that might stress the insertion point.
What kind of drain is used for abdominal surgery
The most common abdominal drains are closed suction systems such as the Jackson Pratt JP drain and the Hemovac. These devices use a bulb or a spring loaded container to create suction that gently removes fluid from the abdomen while minimizing exposure to air. They are typically small bore silicone or flexible latex tubes that exit through a separate stab wound or incision near the operative site. In some situations a passive drain, historically known as a Penrose or Blake drain, may be used, relying on gravity to drain fluid without suction. Passive drains are less common for major abdominal work but may be chosen for specific anatomy or surgeon preference.
Drain types are selected based on expected drainage and tissue tolerance. Closed suction drains generally offer more reliable control of fluid removal and monitoring. The material and size are chosen to minimize tissue irritation while maintaining patency. Drainage color and consistency provide clues about healing. Drain Guide analysis shows that Jackson Pratt and Hemovac types are widely used for many open or extensive abdominal procedures, with surgeon preference playing a role alongside patient factors. The choice of drain is a balance of safety, drainage needs, and comfort during recovery. Drain Guide Analysis, 2026.
How surgeons decide which drain to use
Choosing a drain depends on several practical factors. The surgeon considers the type of abdominal procedure—open versus laparoscopic—as well as the expected amount of tissue disruption and fluid production. In open surgeries with larger spaces to drain, a closed suction system (JP or Hemovac) is often preferred because it provides consistent suction and easier monitoring. For procedures with lower anticipated drainage, or in teaching settings where minimal hardware is desired, a passive drain might be used.
Other considerations include the drain’s position relative to critical vessels and organs, the patient’s overall health, and the risk of infection. If a patient has a higher risk of bleeding or seroma formation, a suction drain may be favored to actively remove accumulating blood. Conversely, if the tissue is fragile or there is concern about suction-related tissue injury, a gentler or passive approach might be chosen. Drain Guide analysis emphasizes that the best choice balances effective drainage with patient comfort and mobility, and that daily drain output informs future decisions about removal.
How drains are managed after surgery
Managing a drain involves a combination of daily observation and basic care. The collection bag or bulb must be kept below the level of the surgical site to promote proper drainage and reduce backflow. Health care teams document the volume and color of drainage each shift, which helps detect early signs of problems like excessive bleeding or infection. The dressing around the exit site should stay clean and dry, and the drain should be secured to prevent accidental pulling.
If the drain is connected to suction, the clinician will check the suction device regularly and ensure that it is functioning correctly. Patients should avoid tugging on the tube, avoid sleeping on the drain side, and follow activity restrictions given by their surgeon. If drainage suddenly increases, changes color, or develops a foul odor, contact the medical team promptly. Regular checks reduce the risk of blockage and ensure the drain continues to work as intended. In many cases, education about self-care and drain care routines helps patients participate actively in their recovery.
Placement sites and care routines
Abdominal drains exit through a small incision near the operative site, often in the lower abdomen or near the incision line. The location is chosen to maximize drainage while minimizing discomfort and risk to nearby structures. Care routines focus on keeping the exit site clean, monitoring for redness or swelling, and ensuring the drain tubing is not kinked or compressed.
Your medical team may offer specific instructions on showering, activity level, and wound care during drain use. Dressing changes are typically performed by nurses or physicians, with patients asked to report any loosening of the dressing. If the drain is secured with sutures or adhesive devices, follow the guidance on how to recognize signs of loosening or migration. Clear, consistent communication with your care team reduces the risk of complications and speeds up recovery.
Potential risks and signs of complications
While drains support healing, they carry potential risks. Infection around the exit site is a common concern and may present as warmth, redness, or increased drainage with a foul odor. Blockage or dislodgement of the drain can reduce efficiency and require repositioning or replacement. Prolonged drainage, especially of blood, can indicate ongoing bleeding or seroma formation. Rarely, drains may contribute to fistula formation or skin irritation from the tube or adhesive.
Be mindful of new or worsening symptoms such as fever, intense local pain, swelling beyond the exit site, or fatigue that accompanies drainage changes. If you notice skin breakdown around the tunnel or a dramatic change in drainage amount, contact your surgeon promptly. Timely reporting and assessment are essential for safe recovery.
Removal, recovery, and when to contact your surgeon
Drain removal is a planned step in the recovery trajectory and occurs when healing progresses and drainage volume remains low or non existent for a defined period. The surgeon or nurse will often remove the drain during a brief procedure or in the clinic setting. Some patients experience mild throbbing or a small wound at the exit site after removal, but pain generally subsides quickly with normal care.
After removal, activity levels can typically be increased gradually as directed by the care team. Monitoring continues because a small amount of serous fluid may temporarily persist at the incision site, which should resolve with time. The Drain Guide team emphasizes tailoring removal timing to the individual patient’s healing and comfort, and to seek help if fever, redness, or increasing drainage recurs after removal.
Got Questions?
What is the purpose of a drain after abdominal surgery?
A drain helps remove excess fluids and air to prevent collections that slow healing or cause infection. It also provides a way for clinicians to monitor the healing process. Drains are tailored to the procedure and patient risk.
A drain after abdominal surgery removes fluids and air to help healing and lets doctors monitor recovery.
What are the common types of abdominal drains?
The most common are closed suction drains such as Jackson Pratt and Hemovac. Passive drains like Penrose are used less frequently. The choice depends on the expected drainage and surgical factors.
Common abdominal drains are Jackson Pratt and Hemovac, with passive drains used in select cases.
How long does a drain stay in place after abdominal surgery?
Duration varies by procedure and drainage. Most drains stay until output decreases to a safe level and the surgeon confirms healing is progressing; this can range from a few days to about a week or more in some cases.
Drains stay until drainage is low and healing shows steady progress, usually a few days to a week.
Can I shower with a drain in place?
Showering depends on the drain type and surgeon guidance. Usually you can bathe or shower with the drain protected and the exit site clean and dry, but follow specific wound care instructions.
Ask your care team before showering; many patients shower with the drain protected and exit site clean.
What are signs of drain problems I should watch for?
Watch for fever, increasing pain, redness around the exit site, foul-smelling drainage, or sudden changes in drainage volume or color. Report these to your surgeon promptly.
Look for fever or red, foul smelling drainage and tell your doctor right away.
When can I resume normal activities after drain placement?
Return to normal activities gradually as advised by your surgeon. Start with light duties, avoid heavy lifting, and follow any restrictions on bending or twisting to protect the exit site and underlying tissues.
Resume activities gradually as advised, avoiding heavy lifting until cleared by your surgeon.
The Essentials
- Follow your surgeon’s drain care instructions exactly.
- Expect drainage to be monitored for color and volume daily.
- Common drains include JP and Hemovac with closed suction.
- Removal happens once drainage is consistently low and healing is adequate.
- Notify the team for infection signs or sudden drainage changes.
- Discuss activity limits and showering with your care team.