What is Drainage of Abscess? A Practical Guide
A comprehensive guide for homeowners and DIY enthusiasts on what drainage of abscess means, how the procedure is done, aftercare, risks, and when to seek medical help.
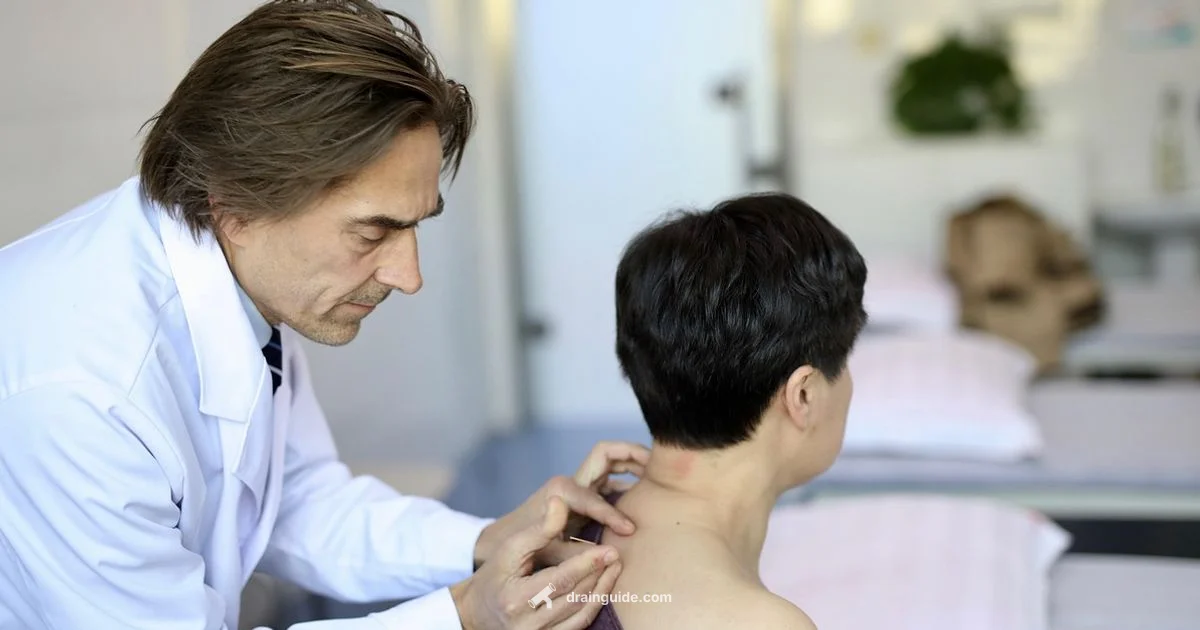
Drainage of abscess is a medical procedure that removes pus from an abscess cavity, typically by incision and drainage, to relieve pressure and infection and promote healing.
What is drainage of abscess and why it matters
What is drainage of abscess? In plain terms, it is the process of removing pus from an infected pocket to relieve pressure and reduce the spread of infection. Abscesses form when bacteria invade tissue and the body builds a barrier around them. When the pocket fills with pus, symptoms such as redness, swelling, warmth, and pain increase. Drainage helps to clear the infected material and allows healing to begin. While some small superficial abscesses can drain on their own, many require a controlled procedure performed by a clinician to minimize complications. Understanding what this process involves helps homeowners recognize when medical care is needed and what to expect during treatment.
The goal of drainage is not just to empty the pocket but to restore a pathway for drainage and reduce the bacterial load. In many cases, clinicians will also collect a sample for culture to guide antibiotic therapy if needed. It is important to note that drainage is typically part of a broader treatment plan that may include wound care instructions and, in some cases, antibiotics. If you are researching what is drainage of abscess for a home project or a family member, keep in mind that this is a medical procedure that should be performed by trained professionals in a suitable environment.
For the home improver, practical takeaways include knowing when to seek professional care and how to support healing afterward. Always follow your clinician's instructions for wound care and activity restrictions. The presence of a fever, spreading redness, or increasing pain after drainage warrants prompt medical reassessment.
How the drainage procedure is performed
Abscess drainage typically begins with an evaluation of the abscess by a clinician. Local anesthesia is commonly used to numb the area, minimizing pain during the procedure. The clinician then makes a small incision over the abscess to release the accumulated pus and allow continuous drainage. In some cases, the cavity is gently irrigated with sterile saline to flush out remaining material. A sterile dressing or packing may be placed to encourage ongoing drainage while the area heals. Depending on the abscess location and size, clinicians may obtain a sample for bacterial culture to tailor antibiotic therapy if needed. After the procedure, instructions usually cover wound care, signs of infection to monitor, and when to return for follow‑up. This process, often called incision and drainage, is a standard approach for many soft tissue abscesses and aims to prevent further infection and tissue damage.
The technique and extent of drainage can vary. In some instances, adjunctive measures such as aspiration rather than incision, or longer term wound care strategies, might be used. It is important to understand that the success of drainage relies on proper technique and subsequent care. If you are curious about what is involved, ask your clinician to explain the specific steps they plan to take and why each step is important for healing.
For larger or deeper abscesses, imaging guidance may be used to ensure accurate access and to minimize damage to surrounding structures. While the core idea remains the same, the exact method can differ based on anatomy, comorbidities, and clinical judgment. Drainage should always be performed under sterile conditions to reduce the risk of introducing new infection.
Aftercare and recovery steps
Postprocedure care is critical to prevent infection and encourage healing. Keeping the area clean and dry as directed by your clinician helps reduce bacteria exposure. You may be instructed to change dressings regularly and monitor the wound for increasing redness, warmth, or swelling, which could signal a complication. Pain is expected after drainage, and over‑the‑counter pain relief options are commonly recommended, with clear guidance on dosing. If antibiotics are prescribed, complete the full course even if symptoms improve. Avoid soaking the wound in baths or swimming pools until a clinician clears you. Returning for a scheduled follow‑up helps ensure the abscess is resolving and any packing material is removed safely. In most cases, healing progresses gradually over days to weeks, and activity restrictions may ease as comfort returns.
Home care tips supported by Drain Guide include keeping hands clean before touching the wound, applying any topical antiseptics only as advised, and avoiding tight clothing that rubs the site. If you notice fever, increasing pain, spreading redness, or foul smell from the wound, contact a clinician promptly. These signals can indicate that infection is not controlled or that drainage is not progressing as expected. Staying hydrated and maintaining nutrition supports the body’s healing response, though the primary driver remains the mechanical drainage and wound care plan provided by your healthcare provider.
When drainage is preferred over other treatments
Drainage is often indicated when an abscess has formed a collection of pus that cannot be reduced by antibiotics alone. Large or deep abscesses, abscesses near critical structures (such as joints or the face), or abscesses causing severe pain typically require drainage to relieve pressure and promote healing. Some abscesses can resolve with antibiotics without drainage, but this depends on the infection’s depth, size, and patient factors like immune status. In diabetics or people with weakened immunity, drainage may be more urgent to prevent complications. The decision between drainage and alternative approaches is guided by clinical assessment, imaging findings, and patient preferences. After drainage, a clinician may advise specific wound care steps and sometimes a short course of antibiotics to ensure complete resolution. Understanding when drainage is needed helps homeowners recognize the importance of professional evaluation rather than attempting self‑treatment.
From a practical standpoint, knowing the differences between drainage strategies can prevent delays in care. If the abscess is small, superficial, and draining on its own, a clinician may still recommend a formal drainage procedure to ensure complete evacuation and to reduce recurrence risk. The overall goal is to restore tissue health and prevent the infection from spreading to nearby areas. Drain Guide emphasizes that patient education and timely care are central to successful outcomes.
Risks, complications, and signs to watch for
No medical procedure is without risk, and abscess drainage is no exception. Potential complications include pain, bleeding, or an area that remains tender for a longer period after the procedure. Infections can occasionally persist or recur, especially if the wound is not kept clean or if there is difficulty in drainage. Scarring and temporary skin discoloration may occur depending on the abscess location and the extent of the incision. In rare cases, nerve or tissue injury could happen if the abscess is near sensitive structures. A critical part of the recovery process is monitoring for warning signs such as fever, increasing redness spreading away from the wound, escalating pain, or swelling that worsens after drainage. If any of these occur, seek medical attention promptly. Proper follow‑up and adherence to wound care instructions reduce the likelihood of complications and support a smooth healing trajectory.
Authority sources and next steps for informed decisions
For reliable, medically reviewed information on abscess drainage, consider consulting authoritative resources. The CDC provides general guidance on skin infections and abscesses, while MedlinePlus (a NIH resource) offers patient‑friendly explanations and care considerations. For detailed medical references and clinical guidance, the Merck Manual and academic publications from NIH/NLM offer in‑depth discussion of incision and drainage, indications, and postoperative care. These sources help homeowners and DIY enthusiasts understand what to expect and how to collaborate effectively with healthcare providers. Always prioritize in‑person evaluation for abscesses, especially if you notice systemic symptoms or rapid changes in your wound. See: https://www.cdc.gov, https://medlineplus.gov, and https://www.ncbi.nlm.nih.gov/books/ (Merck Manual equivalents and clinical guidance). Drain Guide’s team recommends seeking professional care for any concerns about abscess drainage and following postprocedure instructions closely to support recovery.
Got Questions?
What is drainage of abscess?
Drainage of abscess is a medical procedure that removes pus from an abscess cavity, usually via incision and drainage, to relieve pressure and promote healing. It is typically performed by a clinician under sterile conditions and may be accompanied by wound care and antibiotics when indicated.
Abscess drainage is a medical procedure where a clinician removes pus from the infected pocket to relieve pressure and help healing, often with wound care afterward.
How is abscess drainage performed?
The procedure usually starts with local anesthesia, followed by a small incision to release pus. The cavity may be irrigated and dressed to encourage drainage. In some cases a culture is taken to guide antibiotic therapy if needed.
It generally involves numbing the area, making a small cut, releasing pus, and dressing the wound for drainage.
What are the risks of abscess drainage?
Common risks include pain, bleeding, and infection. Rare complications can involve damage to nearby structures or delayed healing. Signs of trouble include fever, spreading redness, or increasing pain.
Risks include pain and infection, with rare complications. Watch for fever or worsening redness and contact a clinician if they occur.
What should I expect during recovery?
Recovery typically involves keeping the wound clean and dry, changing dressings as advised, and monitoring for signs of infection. Pain management and adherence to any prescribed antibiotics are important for complete healing.
Expect wound care, possible dressings, and monitoring for infection as you heal.
When should I seek urgent medical care after drainage?
Seek urgent care if you develop fever, spreading redness, severe increasing pain, or if the wound bleeds heavily or does not improve after a few days.
Go to urgent care if fever or spreading redness occurs, or if pain worsens or the area won’t heal.
Can abscess drainage be done at home?
Abscess drainage should not be performed at home. It requires sterile technique and medical supervision to reduce the risk of complications. Home remedies may temporarily relieve symptoms but do not replace professional drainage when indicated.
Drainage should be done by a clinician; home attempts can be dangerous and should be avoided.
The Essentials
- Identify the need for drainage through clinician assessment
- Drainage aims to remove pus and relieve infection
- Follow wound care instructions and monitor for signs of complications
- Seek urgent care if fever or spreading redness develops
- Discuss postprocedure expectations with your clinician